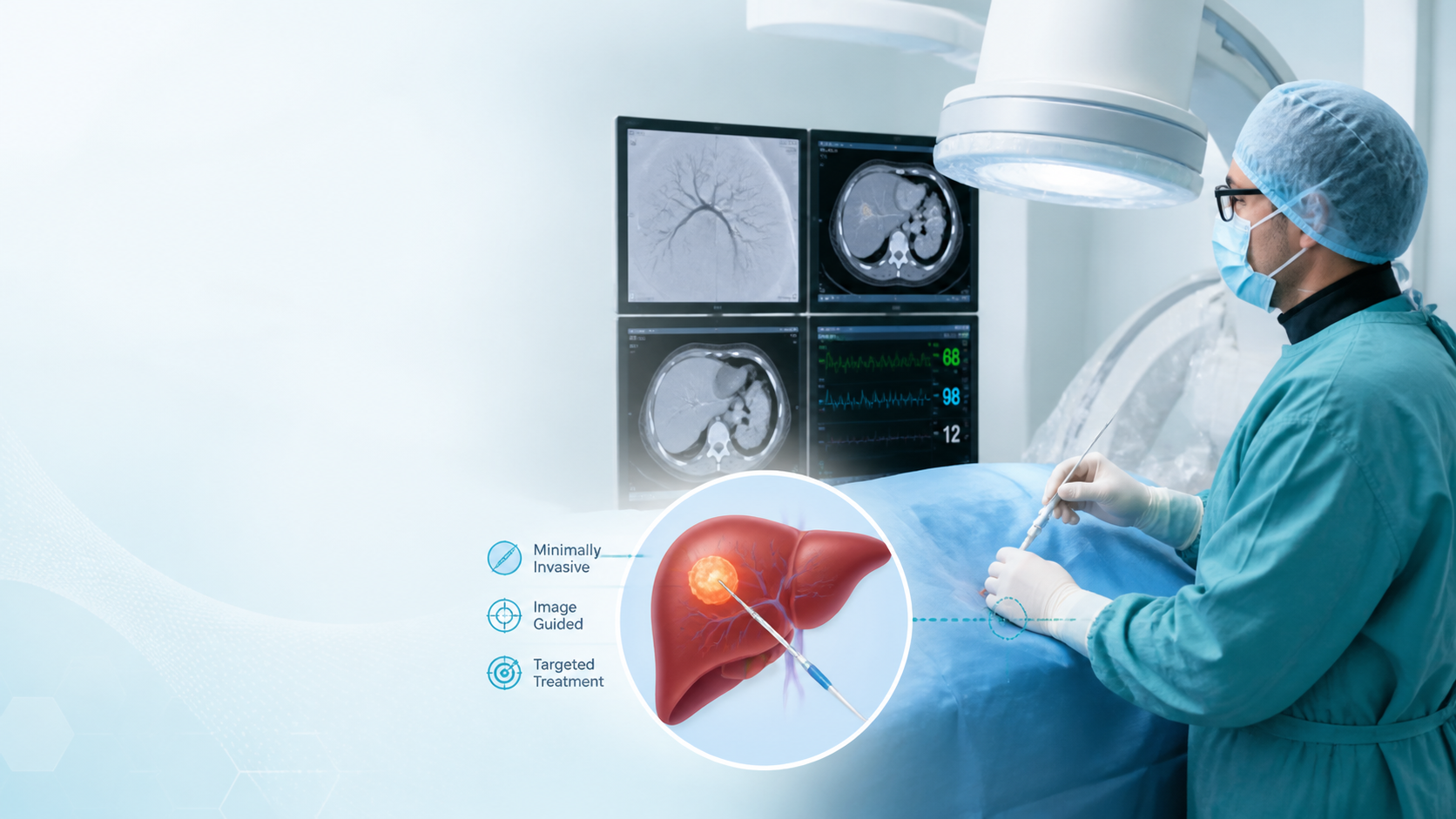
Liver cancer does not always need a large operation to be treated. In many patients, interventional radiology offers a precise, minimally invasive way to target the tumor while protecting healthy liver tissue. This approach is now an important part of modern liver cancer care, especially for patients who are not candidates for surgery.
Why liver cancer treatment needs a smarter approach
The liver is a vital organ, and many patients with liver cancer already have underlying liver disease such as cirrhosis. That means treatment must do two things at once: control the cancer and preserve as much liver function as possible. Interventional radiology is designed for exactly that balance because it treats the tumor directly using image guidance.
What interventional radiology does for liver cancer
Interventional radiologists use ultrasound, CT, MRI, and X-ray guidance to reach the tumor through a tiny skin puncture. Instead of removing large amounts of tissue, they can deliver treatment right into the cancer or its blood supply. This can reduce recovery time, lower procedure-related discomfort, and limit damage to the rest of the liver.
Key interventional radiology treatments
- Ablation for small tumors
Ablation destroys the cancer using heat or other energy delivered through a needle. It is often used for smaller tumors and can be a strong option when surgery is not possible or not ideal.
- TACE to block tumor blood flow
Transarterial chemoembolization, or TACE, delivers chemotherapy directly into the artery feeding the tumor and then blocks that blood supply. This concentrates treatment in the cancer and is commonly used for patients with unresectable or intermediate-stage hepatocellular carcinoma.
- TARE with targeted radiation
Transarterial radioembolization, or TARE, uses microscopic beads carrying radiation to treat the tumor from inside the blood vessels. It is a valuable option in selected patients and may be considered when other liver-directed treatments are less suitable.
Who may benefit most
These treatments are often considered for hepatocellular carcinoma, the most common type of primary liver cancer. They may also be used as a bridge to transplant, as part of a combined treatment plan, or when surgery is not possible because of tumor location, liver function, or overall health. Choosing the right treatment depends on the tumor burden and the condition of the liver itself.
What recovery usually looks like
Most interventional radiology procedures are done through a small puncture, often with sedation or local anesthesia. Many patients return home the same day or after a short stay, though temporary fatigue, pain, nausea, or low-grade fever can happen after embolization-based treatments. Follow-up imaging is essential to measure response and decide whether additional treatment is needed.
Why patients should know about this option
Public awareness of interventional radiology is still limited, even though these procedures are now central to liver cancer care in many hospitals. More patients should know that liver cancer treatment is not limited to open surgery or pills; in the right situation, image-guided therapy can offer a powerful, targeted alternative.
Interventional radiology has changed the way liver cancer is treated. By offering minimally invasive, image-guided therapy, it helps doctors control tumors while preserving liver function and improving quality of life in selected patients.